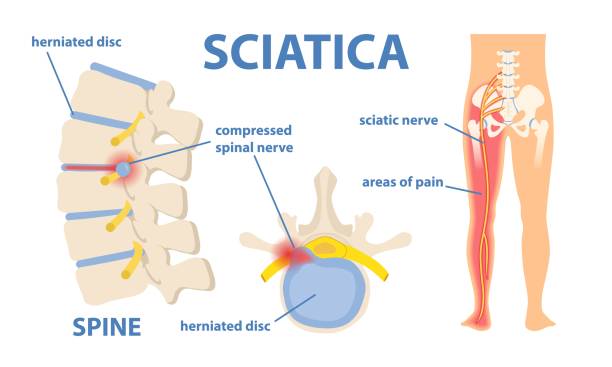
Sciatica can be one of the most painful conditions people experience. Many patients arrive in my clinic barely able to walk, sit, or even stand upright.
A common question people ask is:
“Will chiropractic actually help sciatica?”
The short answer is yes — in many cases it can help significantly, but it depends on the underlying cause of the sciatic nerve irritation.
As a structural, evidence-based chiropractor, I treat sciatica regularly using techniques such as Diversified adjustments, flexion-distraction, SOT (Sacro-Occipital Technique), Activator methods, Torque Release Technique, Neuro Impulse Protocol and soft-tissue work. From my clinical experience, around 80–90% of patients improve with appropriate care.
However, to understand why chiropractic may help, it’s important to first understand what sciatica actually is.
Sciatica is not a diagnosis itself. It is a symptom caused by irritation or compression of the sciatic nerve or its spinal nerve roots.
Typical symptoms include:
Pain radiating from the lower back into the buttock or leg
Tingling or numbness down the leg
Weakness in the leg or foot
Pain that worsens with sitting or bending
The most common causes include:
Lumbar disc bulges or herniations
Piriformis syndrome
Spinal joint dysfunction
Lumbar spinal stenosis
Because sciatica has several different causes, treatment must match the cause.
In many cases, sciatica is related to mechanical pressure on a spinal nerve — often from a disc bulge or spinal joint dysfunction.
Chiropractic care focuses on restoring proper movement and reducing pressure on the nerve.
Depending on the cause, treatment may include:
If a disc bulge is irritating a nerve, techniques such as:
Flexion-distraction
SOT blocking
Manual spinal adjustments
can help reduce mechanical stress on the disc and improve spinal movement.
When sciatica is caused by a tight piriformis muscle, treatment usually focuses more on:
Soft tissue therapy
Stretching
Muscle strengthening and balance
A good example of how quickly sciatica can improve with the right treatment involved a 43-year-old carpenter.
He bent down to pick up a plank of wood and felt a sudden “twinge” in his back. Within 24 hours he developed severe pain radiating down both legs, along with numbness in the right thigh.
He could barely walk due to the pain.
A CT scan confirmed an L4/L5 disc bulge.
Treatment began with:
Flexion-distraction
SOT blocking
Once symptoms improved, we introduced manual adjustments.
His symptoms improved rapidly and he recovered within one week.
Not every case improves that quickly, but this illustrates how mechanical treatment of the spine can relieve nerve irritation when the cause is disc-related.
There is scientific evidence supporting spinal manipulation for some cases of sciatica.
A randomized controlled trial published in the The Spine Journal investigated spinal manipulation for patients with sciatica caused by disc protrusion.
Researchers randomly assigned 102 patients to receive either spinal manipulation or simulated manipulation.
The results showed:
55% of the manipulation group became free of radiating leg pain
compared with 20% in the control group.
Patients receiving manipulation also experienced:
fewer days with pain
lower pain scores
reduced use of pain medication.
Another clinical trial in the Journal of Manipulative and Physiological Therapeutics evaluated spinal manipulation alongside other treatments for sciatica and found meaningful improvements in pain and disability scores over the treatment period.
These studies support what many chiropractors observe clinically — mechanical treatment of the spine can help relieve nerve irritation in appropriate cases.
Chiropractic is not the right solution for every case.
Patients should be referred for medical care if there are signs of:
Severe or progressive neurological loss
Loss of bowel or bladder control
Significant muscle weakness
Disc extrusion or conditions requiring surgery
Chiropractic care also cannot reverse permanent nerve damage.
Responsible clinicians should recognize these red flags and refer patients when necessary.
One of the most common mistakes I see is people trying to relieve pain by lying on their back with their legs up on a chair or sitting in a hot bath in a curled “C-shaped” position.
This may temporarily reduce pain, but it often pushes the disc further backward, increasing pressure on the nerve.
I’ve received many calls from people who did this and then couldn’t get up off the floor afterwards because the pain worsened.
Temporary pain relief is not always the same as improving the underlying problem.
Early movement is usually helpful.
In many cases I recommend:
Gentle walking
Guided stretching
Gradual strengthening once pain improves
The goal is to restore spinal movement and build resilience, not just mask pain.
Unless sciatica occurs after a major accident, disc problems usually develop slowly over time.
They often reflect:
long-term postural stress
poor spinal mechanics
lack of strength or stability
The sudden pain people feel when bending or lifting is often the final straw rather than the true cause.
Addressing those underlying issues is key to preventing recurrence.
So, will chiropractic help sciatica?
Often yes — but it depends on the cause.
Chiropractic care can be effective when sciatica is caused by:
disc bulges
spinal joint dysfunction
muscular imbalance
But some cases require medical treatment or surgery.
The most important step is a proper assessment to determine the real cause of the sciatic nerve irritation.
Valter Santilli et al. Chiropractic manipulation in the treatment of acute back pain and sciatica with disc protrusion: a randomized double-blind clinical trial. The Spine Journal.
Gert Bronfort et al. Spinal manipulation, epidural injections, and self-care for sciatica. Journal of Manipulative and Physiological Therapeutics.
What is the difference between Dry needling, compared to Acupuncture?
We have been asked this question in the clinic many times over the years, so hopefully we can help clear things up in this email;
Dry needling and acupuncture both involve puncturing the skin with thin needles for therapeutic purposes. While a shared aim is to provide relief from pain, the practices are otherwise very different.
Acupuncture is an ancient technique developed in China and there is a wide body of research supports the use of acupuncture to treat many medical conditions.
Proponents state that it can relieve stress, pain, and discomfort by opening up a person’s energy flow, or chi.
Medical acupuncture involves using long, thin needles to stimulate nerves in the muscles and under the skin, which can result in the production of endorphins, which can alleviate a wide range of symptoms
Currently there is strong evidence supporting the effectiveness of acupuncture in conditions such as:
Dry needling is performed by Dr Luke and Dr Regan at the clinic, it is a treatment used by trained practitioners certified in the procedure. The needle penetrates the skin and treats underlying muscular trigger points for the management of neuromusculoskeletal pain and movement impairments. A trigger point is a local contracture or tight band in a muscle fibre that can disrupt function, restrict range of motion, refer pain or cause local tenderness. When dry needling is applied to a dysfunctional muscle or trigger point, it can decrease banding or tightness, increase blood flow, and reduce local and referred pain.
As you can see, these techniques can have very different purposes, and both are a fantastic tool to help you on your particular healing journey.
Like to book a session?
Simply click the button below to be taken to our online booking platfom where you can select a date and time to best suit your schedule.